
(May 16, 2023): The Medicare program is enormous. The Centers for Medicare & Medicaid Services (CMS) estimates that Medicare Administrative Contractors (MAC) process 1.2 billion[1] fee-for-service claims each year in connection with the original[2] (or traditional) Medicare program. If you have ever been involved in a Medicare postpayment audit (or even a prepayment audit[3]) where one or more claims for payment have been denied, you may have decided to challenge the denial through Medicare’s administrative appeals process. The Medicare administrative appeals process allows Medicare providers and suppliers to challenge unfavorable decisions made in connection with traditional Medicare claims for services and supplies.[4] The process involves five levels of appeal, each with specific rules and timelines.[5]
- Level 1: Redetermination Appeal – Medicare Administrative Contractor (MAC).
- Level 2: Reconsideration Appeal – Qualified Independent Contractor (QIC).
- Level 3: Administrative Law Judge (ALJ) Appeal.
- Level 4: Medicare Appeals Council Review (Council)
- Level 5: Federal District Court Review.
I. Most Providers Do Not Appeal Past the Reconsideration Level:
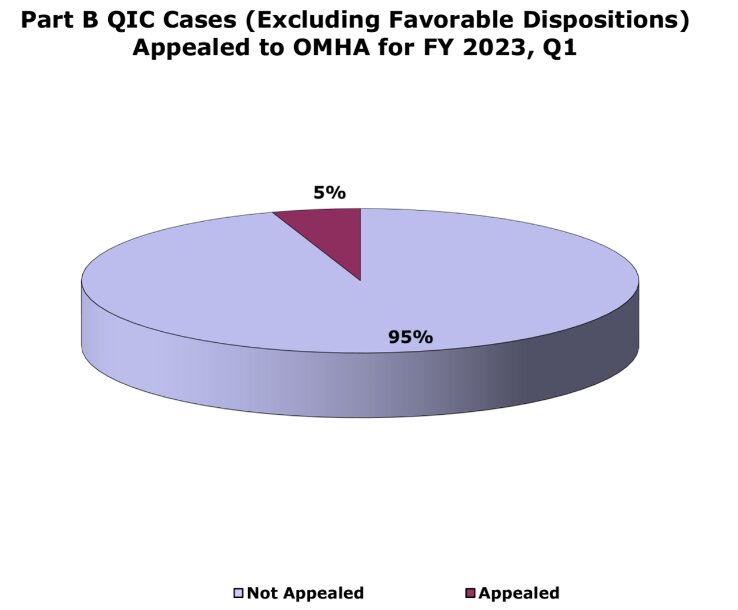
It is important to note that most Medicare providers and suppliers appealing claims denials throw in the towel after the Reconsideration level of appeal and do not appeal any remaining denied claims to the ALJ level. In fact, as of the end of the first quarter FY 2023, it has been reported that 95% of providers who did not prevail at the Reconsideration level of appeal chose NOT to appeal the decision to the ALJ level. There are a number of reasons why the vast majority of providers chose not to pursue their claims further:
First, the appeals process can be lengthy and resource-intensive for healthcare providers. Appealing a denied Medicare claim involves gathering and submitting supporting documentation. Should a provider fail to submit claims related documentation in a timely fashion, it can be very difficult to have the evidence admitted into record after the Reconsideration decision has been issued. Additionally, although the ALJ hearing process is intended to be “non-adversarial”, it can be quite taxing – especially when one or more CMS contractor representatives choose to attend the hearing to defend their findings. In light of the complexities involved, when the alleged overpayments are significant, health care providers and suppliers typically choose to be represented by experienced legal counsel in ALJ hearings.
Second, despite the fact that the Office of Medicare Hearings and Appeals (OMHA) has made significant progress in reducing the ALJ case backlog, many providers are hesitant to get involved in another multi-year case hearing delay. To their credit, the OMHA has made great strides in reducing the case backlog in 2023. Unfortunately, the way the system is currently structured, providers and suppliers cannot further postpone recoupment -- 30 days after a reconsideration decision has been rendered by a Qualified Independent Contractor (QIC), any remaining alleged overpayment is subject to recoupment.
Third, providers and suppliers appealing single claims may not meet the amount in controversy threshold requirements to qualify to advance the appeal to the ALJ level. For calendar year 2023, to meet the jurisdictional requirements, at least $180 must remain in controversy following the QIC’s decision.[6]
II. It is Harder Than Ever to Prevail at the ALJ Level of Appeal:
Many health care providers and suppliers filing an administrative appeal expect to prevail at the ALJ level of appeal. Unfortunately, that ship has sailed. As the chart below reflects, during FY 2022, ALJs issued "Fully Favorable" decisions in favor of appealing health care providers and suppliers a total of 28% (when looking at appeals) and 13.1% (when looking at the total number of claims). While these figures are looking slightly better during FY 2023 (as of April 4, 2023), the message is clear -- it is more important than ever that you diligently work to present your arguments in support of coverage and payment at the Redetermination and Reconsideration levels of appeal.

III. Overview of the Medicare AdQIC Program:
After an ALJ (or an attorney adjudicator) has either heard your case (or issued findings based on the written record), he or she will issue a decision. OMHA then sends the decision and casefile to an organization known as the “Administrative Qualified Independent Contractor” (AdQIC). Here’s where it can get complicated.
- What happens if an ALJ rules against you? If the ALJ ruled against you, the AdQIC will then forward the decision to the appropriate MAC so that the ruling can be effectuated.
- What happens if an ALJ rules that your claims qualify for coverage and payment? If the ALJ ruled in your favor, depending on the way the decision was structured, there is a good chance that the AdQIC will "refer" to the ALJ’s favorable hearing to the Medicare Appeals Council (Council) for possible review.
- What are the Medicare AdQIC contractor’s duties? It is worth noting that Q2 Administrators does not highlight the contractor’s role as CMS’s de facto appeals unit when challenging favorable ALJ decisions as one of its enumerated duties as a contractor. According to Q2 Administrators, their responsibilities include:
- Developing training and standard work protocols.v
- Analyzing appeal outcomes.
- Recommending improvements to the appeals process.
- Managing case files.
- Coordinating contractor participation in Administrative Law Judge (ALJ) hearings.
- Who owns Q2 Administrators? Until 2020, Q2 Administrators was a wholly owned subsidiary of Maximus Federal Services (Maximus). An unknown buyer acquired Q2 Administrators, LLC from Maximus for $3.3 million on May 1, 2020. Prior to this purchase, C2C Innovative Solutions (C2C) protested the issuance of a task order to Maximus. As the Government Accountability Office (GAO) outlined in its letter dated July 18, 2018, the protester (C2C) described the conflict as follows:
“The SOW [statement of work] duties of the AdQIC conflict with the loyalty they have for their own company or parent company and the duty of objectivity owed to CMS. As the AdQIC, Maximus, is financially motivated to withhold issues regarding its own processing of QIC reconsiderations while at the same time, emphasizing to CMS any discrepancies or aberrancies in the reconsideration processing of its competitors, including C2C’s, or any other non-affiliated QIC’s. Maximus’ selective notifications of questionable processing to CMS tarnish the reputation of their competitors’ and help Maximus gain corporately when the task order is re-competed.” [7](emphasis added).
While these concerns are likely no longer applicable since Q2 Administrators was sold in 2020, the question still remains regarding the earlier extended period when it was owned by Maximus.
IV. Reasons for a Medicare AdQIC Referral to the Medicare Appeals Council:
As discussed above, the AdQIC has the authority to appeal an ALJ’s decision[8] to the Council on behalf of CMS and will typically challenge a decision where:
- An ALJ has invalidated a statistical extrapolation. With few exceptions, providers should expect the AdQIC to refer an ALJ decision if the Court has held that the statistical extrapolation of damages imposed by the contractor is not valid. In recent years, it has become a battle of the experts, with statisticians from each side setting out their arguments in favor or, or against the validity of the calculations.
- An ALJ has ruled in favor of a provider and has waived liability for an overpayment under Section 1879 of the Social Security Act. This statutory provision holds that if a provider did not know and could not reasonably have been expected to know that payment would not be made for such items or services under Medicare, the provider cannot be liable.
- An ALJ has ruled in favor of a provider and has waived liability for an overpayment under Section 1870 of the Social Security Act. This statutory provision holds that if a provider is without fault, AND adjustment or recovery would defeat the purposes of Title II or Title XVII of the Social Security Act AND, would be “against equity and good conscience,” liability may be waived.
- An ALJ has taken a position with respect to coverage and payment that the AdQIC contends is contrary to policy or regulations.
In addition to the summary reasons outlined above, there are a number of specialty providers that have historically been the focus of AdQIC referrals. These include, but are not limited to:
- Ambulance transport services.
- Ambulatory Surgical Center (ASC) services.
- Comprehensive Outpatient Rehabilitations Facility (CORF) services.
- Diagnostic Testing Services.
- Durable Medical Equipment, Prosthetics, Orthotics and Supplies (DMEPOS).
- Home Health services.
- Physician services.
- Skilled Nursing Facility (SNF) services.
V. When is a "Win" Truly a "Win"?
Unfortunately, it is becoming more and more difficult each year to rely on a favorable ALJ ruling. In recent years, the Medicare AdQIC has become more aggressive than ever in challenging holdings with which it disagrees. Retired ALJ Bob Soltis said it best when he wrote:
“The AdQIC’s sanctimonious own motion requests are the epitome of what’s wrong with the government, because some of those requests contradict administrative contractors’ payments of similar claims.”[9]
Judge Soltis is correct – the position taken by an AdQIC may, or may not, be consistent with the guidance and rulings of administrative contractors when assessing the coverage and payment status of similar claims. Unfortunately, once the AdQIC refers a matter to the Council, there is a high likelihood that the Council will either remand the case back to the ALJ for further review OR issue its own unfavorable ruling, thereby overruling the decision of the ALJ. Notably, actions taken by the Council are almost always based solely on the record. There is typically no opportunity for a provider to make a live presentation of its arguments in support of payment.
VI. Planning Ahead:
In light of the above, it is important that your legal counsel plan for beyond the ALJ level when asserting defenses to the government’s arguments. While a number of arguments may be persuasive to an ALJ, the same arguments may also automatically generate a referral by the Medicare AdQIC to the Council. Are your arguments drafted to address potential concerns that may be raised by the Council? When hiring an attorney to handle your Medicare claims case, be sure and ask prospective counsel the following:
- How much of your law practice is devoted to health law issues?
- Please describe the extent of your experience handling large, complex administrative appeals of denied Medicare claims.
- How often have you responded to Medicare AdQIC “referrals” of favorable ALJ decisions to the Council for possible review?
- How often have you handled Council appeals?
- Can you provide provider references?
Hopefully, your practice will not face a large administrative appeal of denied Medicare claims. However, should such an event occur, you need to be ready to respond to the contractor’s audit. While there are no guarantees in this business, knowledge of the rules and experience handling administrative appeals may prove essential to increasing the likelihood of your success.

Robert W. Liles, J.D. is an experienced health lawyer and a former Federal prosecutor. He represents healthcare providers and suppliers around the country in Medicare administrative appeals. Liles Parker attorneys have represented Home Health and Hospice, Ambulance Companies, Physical / Occupational / Speech Therapy Clinics, Nursing Homes, Physician Practices, Psychology Practices, DME Companies and a wide variety of other Medicare Part A and Part B providers. Should your practice or clinic be audited by a UPIC, SMRC or CERT, give us a call for a free consultation. We can be reached at: 1 (800) 475-1906
- [1] HHS Primer: The Medicare Appeals Process can be found at: https://khn.org/wp-content/uploads/sites/2/2016/06/medicare-appeals-backlog-primer.pdf
- [2] As opposed to claims submitted directly to Part C Medicare Advantage and Part D Drug payors.
- [3] For a discussion of the various types of prepayment review (automated edits, new provider edits, provider specific edits, provider specific targeted reviews, referral edits and widespread edits), see out article titled “Prepayment Reviews and Audits of Medicare Claims are Ongoing, Are Your Claims Being Audited?”
- [4] Medicare Advantage claims are subject to a completely different set of rules governing the appeal of denials. Providers and suppliers must comply the instructions set out in the denial letters sent by Part C and Part D payors.
- [5] A more detailed discussion of the Medicare Administrative Appeals process can be found at our article titled “Medicare Administrative Appeals Process -- An Overview.”
- [6] It is also worth noting that the amount in controversy to advance a case for judicial review if $1,850 a year. See 87 Fed. Reg. 59,437, 59438 (September 30, 2022).
- [7] GAO Decision Letter covering file B-416289; B-416289.2, page 20, dated July 30, 2018.
- [8] This does not apply in Part D cases. In those case, the Part D QIC typically files an appeal challenging the ALJ’s decision.
- [9] “How to Handle Your Medicare Hearing,” by Bob Soltis, Retired ALJ. Page 82 (2016).
