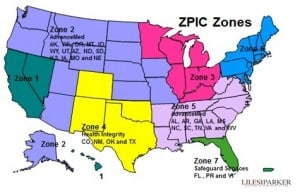
(January 30, 2013): Are the home health services you are currently providing compliant with applicable coverage, documentation and medical necessity requirements? Have you carefully reviewed your current caseload to ensure that each patient does, in fact, qualify as "homebound." Do you have an effective Compliance Plan in place to assist you with your efforts? Now, more than ever before, it is imperative that you understand and follow the rules. Compliance is not optional -- it is required of all participating providers. Home health agencies in Texas, Oklahoma, Alabama, Georgia and Louisiana are under the microscope. "Zone Program Integrity Contractors" (ZPICs), such as Health Integrity and AdvanceMed appear to have increased their use of prepayment reviews in recent months in an effort to identify and prevent the billing and payment of non-covered home health claims. We have received a number of calls regarding the use of this audit tool and have worked with many agencies in an effort to have their prepayment review status reviewed and lifted by the Centers for Medicare and Medicaid Services (CMS). The purpose of this article is to discuss the various types of “prepayment reviews” which may pursued by a CMS contractor.
I. What is a Home Health Prepayment Review?
From a technical standpoint, a prepayment review occurs when the “Fiscal Intermediary Standard System” (FISS System) is programmed by a Medicare Administrative Contractor (MAC) with an “edit” which effectively suspends a claim for further review and assessment prior to deciding whether or not a claim should be paid. Prepayment edits are intended to carve out claims which must be individually reviewed to ensure that the services or supplies at issue qualify for coverage and payment. As reflected below, there are various types and purposes of prepayment edits
- Automated Edits (CMS Pub. 100-08, Ch. 3, §3.3.1.2B). “Automated Edits” are not provider-specific. Rather they are established to carve out any claims which appear on their face to be incorrect. For example, a claim may indicated a “Place of Service” that would be inconsistent with the type of procedure at issue. MACs use a process within the FISS System known as an “Expert Claims Processing System” (ECPS) to set up automated edits. The ECPS reviews claims and decides (based on the edits put into place) whether a claim should be paid, denied or set aside for further review. If a claim is set aside, a request for additional documentation is sent to the health care provider. Once the documentation is reviewed, a payment decision is generally made.
- New Provider/New Benefit Edits (CMS Pub. 100-08, Ch. 3, §3.1B). “New Provider Edits” are typically provider-specific. MACs install these edits to assist in their oversight of new health care providers recently joining the Medicare program as a participating provider. According to at least one MAC, new provider edits are often limited to 20 – 40 claims. This gives MACs and / or ZPICs an opportunity to help ensure that the provider is properly providing and documenting services billed to Medicare. “New Benefit Edits” are typically put into place when a new Medicare program benefit is extended and the MACs need to monitor the new claims to help ensure that they are being provided, documented, coded and billed correctly.
- Provider Specific Probe Edits (CMS Pub. 100-08, Ch. 3, §3.2.2A). “Provider Specific Edits” typically identify specific claims billed by a specific provider and sets them aside for further review prior to payment. Many times, these edits are associated with a specific provider that has experienced a problem before or is suspected of having problems with certain claims for services. When a provider is subjected to a prepayment probe audit, they typically receive written notice of the review. This type of prepayment review can arise out of a complaint by a patient, another provider or even another payor. It may also be generated through data-mining efforts which flag a provider due to their billing patterns. Prepayment probe audits of this type are initially used to examine a relatively small number of claims in order to see if a problem exists. If a problem is identified, the prepayment probe audit may then be expanded to include all claims – this type of prepayment audit is generally referred to as a “Provider Specific Targeted Review” (TR). It may also be extended in duration until the provider can show the MAC or ZPIC that they fully understand the medical necessity and documentation requirements associated with those types of services. When the provider specific probe edits are complete, and it is found that there is a high incidence of inappropriate billing, a provider may be placed on Targeted Review (TR).
- Referral Edits. In some instances, a provider is placed on prepayment review and a “Referral Edit” is put into place. A provider is subjected to a referral edits as a result of a referral from another state or federal government agency. For example, a state surveyor may have identified concerns regarding the quality of care being provided and may have asked a MAC to examine certain services for medical necessity and documentation purposes. If a provider is subjected to a referral edit, they are typically notified in writing that the review is being conducted. They may or may not be advised of the identity of the referring agency.
- Widespread Edits. MACs will typically install a “Widespread Audit” in situations where specific types of claims have been identified through data-mining and other analyses as likely to be problematic. Widespread audits may focus on issues such as:
- Length of stay.
- Number of visits.
- Use of certain modifiers.
- Certain diagnosis codes. For example, edit 5023T selects home health claims for diagnosis 401.9 (Hypertension) and a length of stay longer than 120 days.
- Previous denials for a specific beneficiary. For example, edit 59BY9 selects home health claims due to previous denial related to a specific beneficiary.
- Provider Specific Targeted Review (TR) Edits are implemented against a specific provider. This type of prepayment review is typically initiated by a ZPIC. It may be partial (typically a percentage of the claims billed will be pulled for audit) or it may complete. As you can imagine, this type of prepayment review can wreak havoc on a provider’s finances, depending on their payor mix. Prepayment reviews of this type may be extended in duration.
II. What Should Agencies Expect Targeted Home Health Prepayment Reviews are Initiated?
We have worked with a number of home health providers placed on targeted prepayment review. To be clear, there is no “silver bullet” to getting off of this status and having your payments reinstated. Moreover, there is no administrative appeal process which may be pursued. In our experience, the best and fastest way to get off of prepayment review is to work with professionals who understand the issues. Until a home health agency is able to show a ZPIC that you and your staff fully understand the medical necessity, documentation, coverage, coding and billing requirements applicable to these claims, a targeted prepayment review may last up to a year, or in some cases, even longer. If you need assistance with these compliance issues, give us a call.

Robert W. Liles and other Liles Parker attorneys have extensive experience assisting health care providers placed on prepayment review or subjected to a post-payment audit. Should you have any questions, please call Robert for a free consultation. He can be reached at: 1 (800) 475-1906.
