
(January 22, 2018): The Department of Health and Human Services, Office of Inspector General (HHS-OIG) has conducted numerous audits, evaluations, and investigations involving the provision of "personal care services" to Medicaid beneficiaries. In fact, from 2006 to 2012, HHS-OIG produced more than 20 audit and evaluation reports analyzing various program integrity risks presented when providing personal care services. Much of this work was summarized in a November 2012 report entitled "Personal Care Services: Trends, Vulnerabilities, and Recommendations for Improvement". [1] Additionally, last month, HHS-OIG published an Issue Brief highlighting the involvement of State Medicaid Fraud Control Units (MFCUs) in pursuing health care fraud and beneficiary abuse in personal care services programs.
In this article, we have taken the summary information assembled by HHS-OIG in the reports outlined above and combined this information with data collected from the 50 state MFCUs in order to provide an overview of state and federal investigations, indictments, convictions, and recoveries involving fraud, waste, abuse and patient neglect in Medicaid personal care services programs around the country. Before examining this information, let’s go over a few basics.
I. What Are “Personal Care Services”?
The coverage and scope of a state’s specific personal care services benefit varies from one state’s Medicaid program to another. Using Texas as an example, prior to 2006, personal care services under Medicaid were only provided to qualified minors with physical disabilities and other medical needs. Notably, children with cognitive or behavioral disabilities did not qualify for this benefit. As a result of a class action lawsuit settlement,[2] the Texas Medicaid State plan was amended to cover personal care services for children with disabilities and chronic health conditions enrolled in the state’s Medicaid program. Today, the Texas Department of State Health Services describes “personal care services” as:
“A Medicaid benefit that assists eligible clients who require assistance with activities of daily living (ADLs) and instrumental activities of daily living (IADLs) because of a physical, cognitive or behavioral limitation related to their disability, physical or mental illness, or chronic condition.”[3]
Examples of ADLs that are often provided under the personal care services benefit include bathing, eating, toileting, positioning and transferring, dressing and walking. IADLS provided under the benefit typically include doing laundry, performing light housework, shopping for groceries and preparing meals. As these tasks and activities reflect, personal care services are non-skilled in nature. Skilled services provided by nursing personnel do not qualify as personal care services, though they may qualify under some other benefit such as home health.
It is also important to remember that neither ADLs nor IADLs would qualify as covered personal care services if a beneficiary has the physical, behavioral and cognitive ability to perform these tasks and activities without adult supervision.
II. Who Qualifies for Medicaid-Covered Personal Care Services?
Like the service itself, whether a person qualifies for personal care services depends on the specific requirements of each state program. However, using Texas as an example, a beneficiary must:
- Be 20 years or younger and be eligible for Medicaid.
- Have a disability, physical or mental illness, or a health problem that lasts for a long time.
- Have a Practitioner Statement of Need signed by a practitioner (physician, advanced practice nurse, or physician assistant) who has examined you in the last 12 months.
- Need help with ADLs and IADLs based on the Personal Care Assessment Form (PCAF).
- Provide a reason why your guardian cannot help you with ADLs and IADLs.[4]
III. Trends in Medicaid Personal Care Service and MFCUs:
Between 2012 and 2015, Medicaid spending on personal care services jumped from $10.9 billion to $13.3 billion.[5] As a result, MFCUs have increasingly been tasked with investigating and prosecuting Medicaid provider fraud and patient abuse and neglect within healthcare facilities. Despite being only one of 80 types of providers regulated by MFCUs, personal care service providers constituted 38% of their indictments and 34% of their convictions. During this period indictments and convictions related to fraud by personal care service providers increased 56% and 33% respectively. In the year 2015, cases of fraud by personal care service providers constituted 12% of all MFCU investigations. Overall these trends indicate that MFCUs are concerned with the vulnerability of Medicaid beneficiaries and are more aggressively targeting personal care service providers.
IV. Current Systemic Weaknesses Facilitate Fraud, Abuse, and Neglect:
Throughout last month’s report, HHS-OIG highlighted many of the weaknesses of the current model of Medicaid personal care service oversight. Presently, there are no federal training or educational requirements for personal care service attendants so the quality of personal care services provided from one caregiver to another can vary greatly. Additionally, thorough background checks are not consistently required. As a result, there have been a number of instances where habitual offenders have been found to have exploited beneficiaries under their care.
Another issue of concern is that thorough documentation is not required for Medicaid personal care services, leading to the ability of an attendant to charge for services that did not occur or for time in which the attendant and beneficiary where not even in the same location. Aside from creating a window of opportunity for fraud, this also allows for personal care service attendants to neglect their beneficiaries. In the past, this scenario has led to the death of a beneficiary. Lack of oversight also shifts the burden to report on to the beneficiary. Thus, mental and physical handicaps of beneficiaries leave them vulnerable as reporting may be rather difficult. Due to federal regulations, MFCUs are also unable to investigate or prosecute cases of abuse or neglect by in-home/community personal care service providers.
As a consequence of these systemic issues, despite being the best equipped agency to take on this task, MCFUs do not receive funding for this and are forced to refer such cases to other agencies that may be less effective in investigating and prosecuting these cases. Overall, the current model is vulnerable to fraud and leaves beneficiaries vulnerable to abuse and neglect.
V. Improper Payments to Personal Care Service Providers Will Lead to Investigations:
An improper payment is any payment that is made that, according to federal and/or state laws, should not have been made. The inconsistency in state rules and the lack of depth of federal rules complicates the generalization of improper payments. According to an audit of state Medicaid programs by HHS-OIG, the most common types of improper personal care service payments are:
- Claims paid without supporting documentation.
- Services provided and billed that are ineligible for Medicaid reimbursement.
- Services provided without required supervision.
- Services provided by an unqualified attendant.
- Services provided by an attendant without proper verification of required qualifications.
- Payments made for care while the Medicaid beneficiary was in an institution.
It is important to note that improper payment is not the same as fraud. Improper payments are considered a result of error and a personal care service provider is required to return the overpayment as soon as the improper payment is discovered and may face further consequences. While self-disclosure of improper payments is considered an act of good faith, the nature of the improper payment may lead into an investigation into potential waste, fraud, and/or abuse.[6]
VI. What is Personal Care Services Fraud?
The vulnerability of the current personal care services system to fraud has made these services a significant concern for MCFUs around the country. Many of the fraud cases brought in recent years have involved instances of billing for services not rendered to a Medicaid beneficiary. Examples of this type of improper conduct has included instances when:
- A Medicaid beneficiary was on a vacation.
- A Medicaid beneficiary was in an institution.
- A Medicaid beneficiary was documented to be without the personal care attendant by another healthcare provider.
- The personal care aide or attendant was documented to be working elsewhere at the time.
- The Medicaid beneficiary was deceased at the time personal care services were billed.
Often, wrongdoers have committed this type of fraud by having a Medicaid beneficiary sign off on blank time sheets in advance of services that are to be provided. While the Medicaid beneficiary is typically unaware of the fraudulent intentions of the personal care attendant, there have been cases where the personal care services attendant has made an agreement to share profits with the beneficiary or a family member of the beneficiary in order to obtain a signed blank time sheet.
While fraud is often committed by individual personal care aides or attendants, a personal care services agency can be held accountable if it is aware of the attendant’s fraudulent billing practices. One investigation in Alaska led to the criminal prosecution of over 40 individuals for fraud.[7] In that case, the personal care services agency was aware that employees were submitting falsified timesheets in addition to charging Medicaid for services rendered by excluded individuals.
VII. Personal Care Services Fraud Investigations:
Personal care services fraud has been an increasing concern of MCFUs. As expected, the amount of criminal investigation into personal care services fraud has risen over the 2015 and 2016 fiscal years, with a total of 1,929 individual personal care services attendants and 250 personal care services agencies being investigated for fraud at the end of 2016.[8] Convictions have risen slightly over those 2 years, with 464 individual personal care aides and attendants and 36 personal care services agencies convicted of criminal fraud charges in 2016. Overall, personal care service fraud appears to more commonly perpetrated by individual personal care service attendants, though agencies are certainly being held responsible for their role in personal care services fraud.
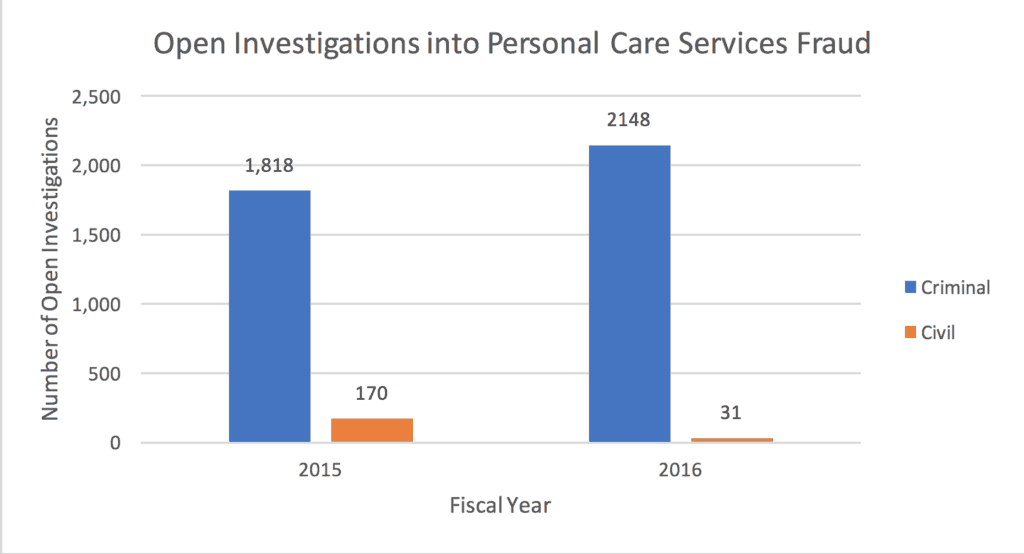
Table 1:
The number of open investigations into personal care services fraud by agencies and attendants at the close of the 2015 and 2016 fiscal years.
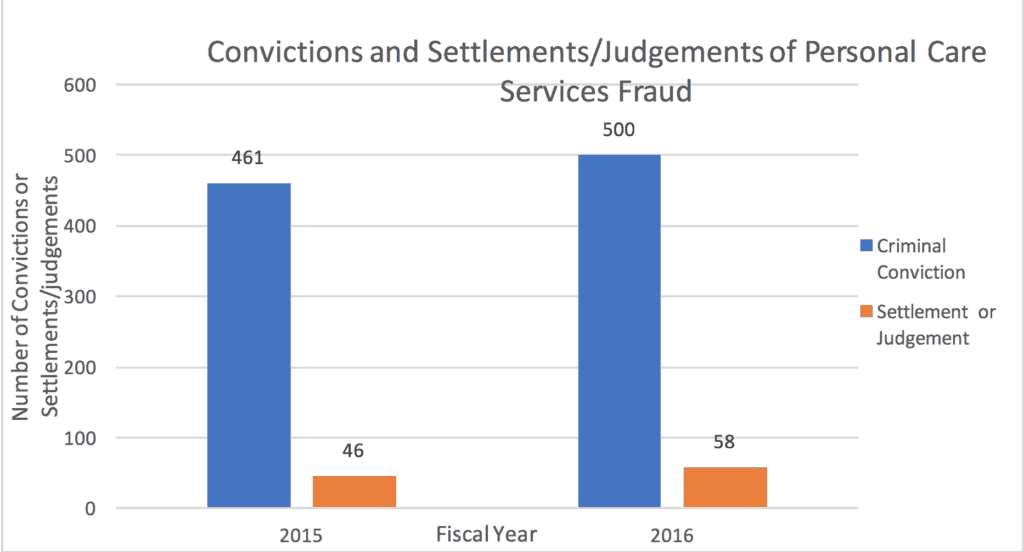
Table 2:
The number of criminal convictions and civil court settlements/judgements for personal care services fraud in the 2015 and 2016 fiscal years.
VIII. Recoveries from PCS Fraud Cases:
Despite an increase in civil settlements and judgements, the total amount recovered through settlements decreased substantially for both PCS attendants and PCS agencies. The result of criminal convictions has been markedly different. In the fiscal year 2016, a total of 464 PCS attendants were convicted of PCS fraud compared to only 36 agencies.[11] While personal care attendants constitute the overwhelming majority of convictions, approximately 45.8% of the amount recovered in 2016 came from personal care service Agencies. From fiscal year 2015 to 2015, the amount of PCS agencies convicted increased by 63.6%, from 22 to 36. In the same period, the amount recovered from criminal convictions of PCS agencies more than doubled, from $1,718,223 to $4,108,575. Thus, it is evident that PCS agencies are increasingly being held responsible for their role in PCS fraud.

Table 3:
The amount of money recovered in personal care services fraud cases in the 2015 and 2016 fiscal years.
IX. What is Abuse or Neglect of a Beneficiary?
The current system leaves beneficiaries vulnerable to abuse. Abuse has cases revolve around incidents in which a personal care services attendant causes physical harm to the beneficiary. In a case in Florida, a personal care attendant was fired and later charged with elderly abuse after repeatedly striking, pinching, and pulling at an elderly individual and leaving bruises on the individual.[13] However, abuse is not always physical. Abuse also includes harm done by theft, in which personal care service attendants take advantage of their beneficiaries and steal valuable items from them. In one case, a personal care service attendant at an assisted living facility stole nearly $10,000 from beneficiaries.[14] In another, an attendant stole two guitars from a beneficiary and sold the guitars to a local music shop.[15] When the attendant became aware of the beneficiary’s intent to contact authorities, the attendant returned the items. In the end, the attendant was still charged with fourth degree larceny.
Drug diversion is a serious abuse prevalent in personal care service that goes beyond theft and extends into physical harm as well. In addition to the monetary loss, the beneficiary is losing the treatment they require. For many, especially in hospice care, the use of opioids is used to manage pain. When attendants take these medications, they leave the beneficiaries suffering. In one case, an attendant began to switch a beneficiary’s hydrocodone with acetaminophen, leaving the patient suffering until the attendant’s drug diversion was discovered. In addition to leaving patients suffering, the use of substitute substances and potentially unsterile equipment puts the beneficiary at risk of serious harm or death.
Neglect is defined as “the failure or omission on the part of a caregiver to provide the care, supervision, and services necessary to maintain the physical and mental health of a disabled adult or elderly person that a prudent person would deem essential for the well-being of the patient.” Neglect is serious, as the lack of adequate care or supervision of vulnerable individuals can be fatal. In one case, a personal care service attendant did not provide the services that were billed for an entire week, leaving the beneficiary hospitalized due to malnourishment and dehydration.[16] In another case, a personal care service attendant took a mentally handicap person to a crowded shopping area and lost the individual on a winter day in Philadelphia. The attendant did not immediately seek out the beneficiary nor did the attendant contact authorities in a prompt manner. The beneficiary was later found dead due to hypothermia. Neglect can also stem from fraud. In one case in Arkansas, a personal care service attendant billed Medicaid for services rendered to a beneficiary while frequenting Casino.[17] The attendant’s neglect led to malnourishment and dehydration, eventually leading to the death of the beneficiary.
X. Investigating Abuse or Neglect of a Beneficiary:
Despite the desire of MCFUs to investigate abuse or neglect, allegations are not investigated as often and extensively as they would like due to a lack of federal and state funding to do so. From the close of the 2015 fiscal year to the close of the 2016 fiscal year, open investigations into Abuse or neglect of a beneficiary decreased marginally from 254 to 252 investigations.[18] This marginal decline indicates the limitations placed on MCFUs ability to investigate abuse or neglect of beneficiaries. All of these investigations were criminal. In the same period, criminal convictions for abuse or neglect raised from 44 in 2015 to 52 in 2016. In 2015, there was one civil court settlement for abuse or neglect by a personal care service attendant. Overall it appears that MCFUs are becoming increasingly serious about addressing abuse or neglect by personal care service attendants and will continue to do what they can within their means to address the issues.
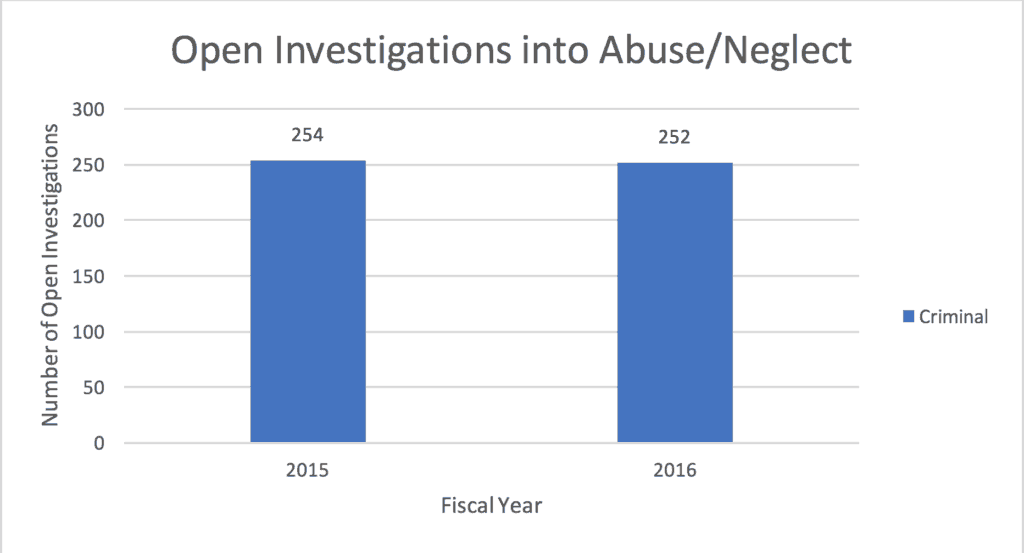
Table 4:
The number of open investigations into abuse or neglect by personal care service attendants at the close of the 2015 and 2016 fiscal years.
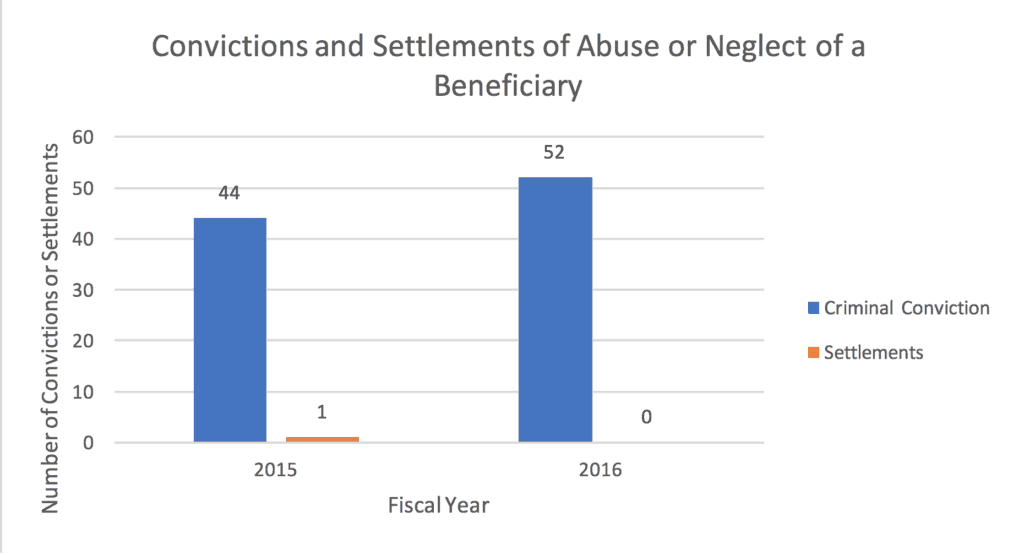
Table 5:
The number of criminal convictions and civil court settlements/judgements for personal care service abuse or neglect cases in the 2015 and 2016 fiscal years.
XI.Recoveries from Abuse or Neglect Cases:
As can be expected by the findings of the recent HHS-OIG issue brief, convictions of abuse or neglect of a beneficiary only increased by 8 convictions in 2016, an 18% increase from the 2015 fiscal year. This again highlights the limitations placed of MFCUs in addressing abuse or neglect of beneficiaries. However, the total amount recovered in these cases more than tripled from the 2015 to the 2016 fiscal year, from $71,817 in 2015 to $247,972 in 2016. This substantial increase in recoveries again suggests that MFCUs are increasingly serious about addressing abuse or neglect of beneficiaries.
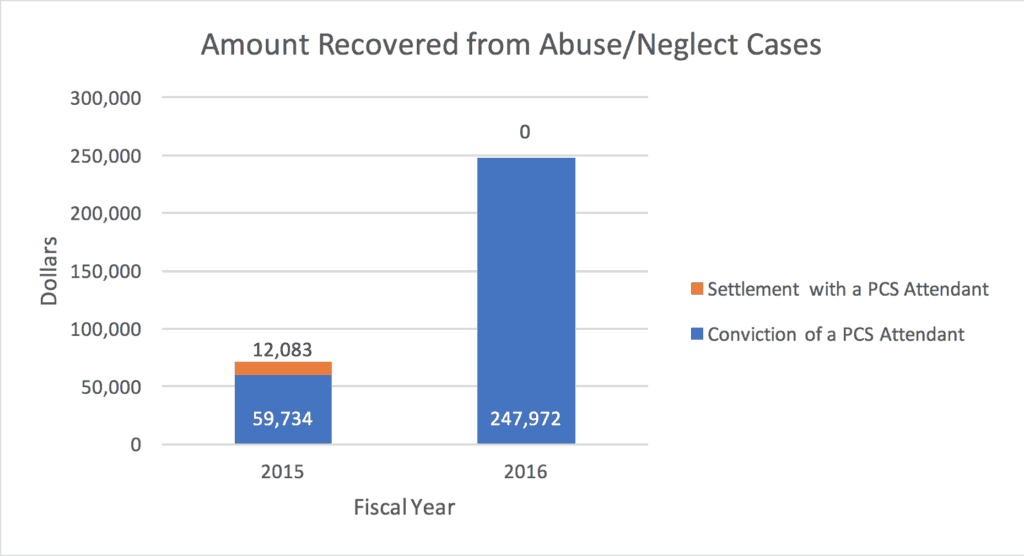
Table 6:
The amount of money recovered in personal care service abuse or neglect cases in the 2015 and 2016 fiscal years.
XII. HHS-OIG Recommendations:
The recommendations made by HHS-OIG are aimed at creating greater state oversight of personal care services provided by aides and attendants to Medicaid beneficiaries. These recommendations include measures such as:
- Creating an enrollment or registration process for attendants.
- Requiring comprehensive background checks for personal care service attendants
- Mandating greater documentation requirements for personal care service attendants, including details such as time of service and services provided.
- Requiring beneficiary case managers to conduct more in-home/community supervisory visits.
- Establishing mandatory training or educational standards for personal care service attendants.
- Cross-referencing personal care service attendant and beneficiary locations to prevent fraudulent billing.
- Federal funding for investigations and prosecutions of abuse or neglect by in-home/community personal care service agencies.
The current model provides too much opportunity for fraudulent, negligent, and abusive behavior by agency providers to be overlooked. These reforms could effectively deter personal care service providers from engaging in fraudulent, abusive, or negligent behavior by making them aware of the consequences of such behavior. In addition, these reforms would make it easier for MFCUs to effectively hold all personal care service providers accountable for their actions.
XIII. Conclusion:
At present, despite efforts from personal care agencies to better screen their staff, Medicaid beneficiaries are still finding themselves subject to fraud, abuse and / or neglect by a significant number of individual personal care service aides and attendants each year. Unfortunately, fraud, abuse and / or neglect by personal care service aides and attendants will likely continue to be a major concern until the further safeguards are taken by both personal care agencies and regulators to better protect Medicaid beneficiaries.
In addition to conducting standard due diligence, as an owner of a personal care services agency, it is especially important that you screen your applicants (before hire), employees, vendors and contractors, against all Federal and State exclusion databases, every 30 days. We recommend that you contact the folks at Exclusion Screening to get this accomplished. They can be reached at www.exclusionscreening.com

- [1] As mandated by Public Law 95-452, HHS-OIG’s mission is to “protect the integrity of the Department of Health and Human Services (HHS) programs, as well as the health and welfare of beneficiaries served by those programs.” HHS-OIG’s report entitled “Personal Care Services: Trends, Vulnerabilities, and Recommendations for Improvement” (OIG-12-12-01).
- [2] Alberto N. et al. v. Hawkins. (No. 6:99-cv-00459) May 19, 2005. EDTX, Tyler Division.
- [3] https://www.dshs.texas.gov/region1/documents/tmp-personalCareservices.pdf
- [4] https://www.dshs.texas.gov/caseman/pcs.shtm
- [5] https://oig.hhs.gov/oei/reports/oei-12-16-00500.pdf
- [6] “Waste” occurs when unnecessary services are provided that lead to a waste of resources, such as when more hours of services are rendered than are necessary. “Fraud” is defined at 42 C.F.R. §433.304 as “(in accordance with §455.2) . . . an intentional deception or misrepresentation made by a person with knowledge that the deception could result in some unauthorized benefit to himself or some other person. This includes any act that constitutes fraud under applicable Federal of State law.” “Abuse” is defined is defined at 42 C.F.R. §455.2 as “provider practices that are inconsistent with sound fiscal, business, or medical practices, and result in an unnecessary cost to the Medicaid program, or in reimbursement for services that are not medically necessary or that fail to meet professionally recognized standards for health care. It also includes beneficiary practices that result in unnecessary cost to the Medicaid program.”
- [7] https://oig.hhs.gov/reports-and-publications/portfolio/ia-mpcs2016.pdf
- [8] https://oig.hhs.gov/oei/reports/oei-09-17-00210.pdfhttps://oig.hhs.gov/oei/reports/oei-07-16-00050.pdf
- [9] Ibid.
- [10] Ibid.
- [11] Ibid.
- [12] Ibid.
- [13] http://www.myfloridalegal.com/newsrel.nsf/newsreleases/8A86BFE3E705BD60852580D5006CC686
- [14] http://www.fox9.com/news/caregiver-admits-to-stealing-thousands-in-cash-jewelry-from-elderly-patients
- [15] https://www.nbcconnecticut.com/news/local/Personal-Care-Attendant-Accused-of-Stealing-Guitars-from-Client-in-Southington-464400253.html
- [16] https://oig.hhs.gov/reports-and-publications/portfolio/ia-mpcs2016.pdf
- [17] http://www.swtimes.com/news/caretaker-arrested-fort-smith-man-s-death?start=6
- [18] https://oig.hhs.gov/oei/reports/oei-09-17-00210.pdfhttps://oig.hhs.gov/oei/reports/oei-07-16-00050.pdf
- [19] Ibid.
- [20] Ibid.
- [21] Ibid.
