(July 16, 2018): Do you provide Transcranial Magnetic Stimulation care and treatment services? If so, you need to ensure that your medical necessity, documentation, coding and billing practices fully comply with applicable statutory, regulatory and administrative guidelines. In recent weeks, a flurry of prepayment review letters from Medicare Administrative Contractors (MACs) have been sent to physicians and health care entities seeking copies of the medical records and related documentation associated with transcranial magnetic stimulation services (also commonly referred to as TMS services). Billed as CPT 90868, transcranial magnetic stimulation services are merely the latest risk area being examined by MACs and the associated Uniform Program Integrity Contractor (UPIC) assigned to a specific jurisdiction of the country.
I. Why Are My Transcranial Stimulation Services Being Audited?
If you received notice of a prepayment or audit of your claims from a MAC or UPIC contractor working for the Centers for Medicare and Medicaid Services, you may have contacted the contractor to find out why your claims were selected for audit. Although the CMS contractor may have advised you that your claims were "randomly" chosen for audit, nothing could be further from the truth. At this time, CMS has not authorized its contractors to conduct random audits of provider claims. As set out in the Federal Register:
"Although section 934 of the MMA sets forth requirements for random prepayment review, our contractors currently do not perform random prepayment review. However, our contractors do perform non-random prepayment complex medical review. We are cognizant of the need for additional rulemaking should we wish our contractors to perform random review." [1]
If your claims were not audited as a result of a random review, then why were your claims selected for prepayment or postpayment review? As set out in the Medicare Program Integrity Manual, Chapter 2, Section 2.4, Subsections A-C, CMS processing and program integrity contractors have been directed to utilize data analyses as their primary tool to identify outliers and other providers that may be engaging in improper, fraudulent, wasteful and / or abusive coding and billing practices. UPICs and other program integrity contractors have more than a dozen various utilization, coding and billing databases at their disposal in this regard. Simply put, your claims were likely chosen for prepayment review because of a specific concern with respect to a type of service or because your utilization of one or more claims differed from that of your peers.
II. Overview of Transcranial Magnetic Stimulation Services:
Transcranial magnetic stimulation involves the noninvasive use of magnetic pulses to stimulate the brain. This treatment protocol involves the positioning of an electromagnetic coil on a patient's scalp. Once properly placed, an electric current is intermittently run through the electromagnetic coil, thereby producing brief magnetic pulses that painlessly pass through a patient's brain. Transcranial magnetic stimulation services are normally conducted in an outpatient setting and do not require anesthesia or analgesia. Although a number of proponents have consistently pressured Medicare to expand its current scope of coverage, at this time, only adults who have a confirmed diagnosis of Major Depressive Disorder, and meet a number of other requirements, qualify for transcranial magnetic stimulation under Medicare's strict medical necessity requirements.
III. Transcranial Magnetic Stimulation Claims Audits:
- MAC prepayment targeting of transcranial magnetic stimulation claims.
Among its many functions, National Government Services (NGS) and other MACs around the country are required to conduct medical reviews of provider claims on a prepayment basis, to better ensure compliance with Medicare's coverage and payment rules.[2] The fact that NGS and other MACs are currently auditing transcranial magnetic stimulation (CPT Code 90868) claims, is significant because MACs are only required to initiate targeted provider-specific prepayment reviews "when there is the likelihood of a sustained or high level of improper payments." [3] It is also worth noting that providers are being directed to submit their supporting documentation directly to the Uniform Program Integrity Contractor (UPIC) assigned to their jurisdiction. - UPIC reviews of transcranial magnetic stimulation claims.
UPICs are private, for-profit companies that awarded contracts to provide program integrity services for the Centers for Medicare and Medicaid Services (CMS). UPICs are tasked with investigating instances of suspected fraud, waste, and abuse in the Medicare and Medicaid programs. Should the UPIC identify possible overpayments, the results of their audits will be sent back to the MAC for recoupment action. However, if evidence of possible fraud is identified, a UPIC may forward their findings to law enforcement for review, investigation and possible prosecution.[4]
IV. Transcranial Magnetic Stimulation Audit Risk Issues (Partial Listing):
If you are providing transcranial stimulation services and billing them to Medicare, you need to keep in mind that the failure to meet the following requirements can quickly lead to an audit of your CPT Code 90868 claims:
- Is the transcranial magnetic stimulation device approved by the Food and Drug Administration (FDA)? In most instances, if a treatment device has not been approved by the FDA, CMS and its contractors will consider the device to be “experimental.” As such, any transcranial magnetic stimulation treatment services performed will not be covered by Medicare.
- Does the patient have a “confirmed” diagnosis of major depressive disorder? For Medicare, this is a deal-breaker. Although a number of studies have been conducted examining the use of this treatment modality in connection with other diagnoses, none of these additional diagnoses are currently covered and will be considered “experimental” by CMS and its contractors. A few examples of diagnoses that will be denied include schizophrenia, schizoaffective disorder epilepsy, cerebrovascular disease, and dementia. Finally, it is important to keep in mind that UPIC auditors will be examining each case carefully to ensure that the diagnosis of major depressive disorder has been fully documented and validated (or otherwise confirmed). UPIC auditors will be looking for assessments of the patient’s condition using standardized rating scales (such as the Beck Depression Scale or the Montgomery-Asberg Depression Rating Scale) that have been found to reliably measure the intensity of a patient’s depressive symptoms. Merely concluding that a patient suffers from major depressive disorder without the test results to support your diagnosis is insufficient to support medical necessity. Finally, under the LCD guidance issued by NGA, once transcranial magnetic stimulation treatment has been initiated, the provider is required to monitor the patient’s treatment response using the standardized rating scales discussed above (or a similar, widely accepted rating scale).
- Transcranial magnetic stimulation treatment sessions must be ordered and supervised by a qualified individual. As LCD L33398 reflects, in order for transcranial magnetic stimulation therapy to be ordered (or reordered), the ordering physician must issue the order in writing. Moreover, the ordering physician must have examined the patient, reviewed the record AND must have experience in administering transcranial magnetic stimulation therapy services. As a final point, the treatment must be given under the direct supervision of the ordering physician. In other words, the physician must be in the area and be immediately available.
- Does your practice also bill for CPT Code 90836 claims? We have seen a higher likelihood of audit if you are also billing CPT Code 90836[4] claims along with your billing of transcranial magnetic stimulation services (CPT Code 90868). It is important to keep in mind that the billing of this “add-on” code may trigger an audit even in the absence of CPT Code 908686 billings. For example, in a September 2016 Medicaid case brought under Connecticut’s False Claims Act, it was alleged that the defendant was billing this “add-on” code for psychotherapy sessions when in fact, she instead provided medication management services, or a brief meeting with the patient for drug change/dosage adjustment.
- Does your practice also bill for CPT Code 99214 claims? Audits of transcranial magnetic stimulation claims have also sometimes included a concurrent review of the provider’s CPT Code 99214 [6] claims. Since at least 2012 the Department of Health and Human Services (HHS), Office of Inspector General (OIG) has expressed its concerns with respect to the unsupported, improper billing of this Evaluation and Management (E/M) code.
V. When Are Transcranial Magnetic Stimulation Services Covered by Medicare?
- “Indications” -- a confirmed diagnosis of Major Depressive Disorder is required for coverage.
Medicare has adopted strict requirements on the coverage and payment of transcranial magnetic services. As set out in the Local Coverage Determination [7] (LCD) guidance published by NGS (LCD L33398) [8], transcranial magnetic stimulation services are only considered medically necessary "in adults who have a confirmed diagnosis of major depressive disorder (MDD), single or recurrent episode." Additionally, in order for the care to qualify for coverage and payment, the record must show: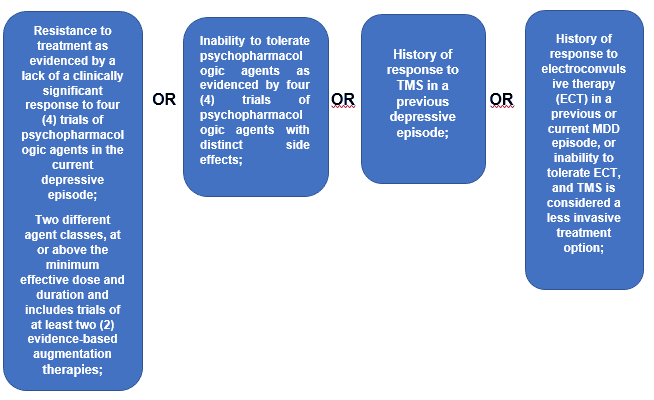
In addition to having a diagnosis of "Major Depressive Disorder," one of the above four conditions must be fully documented in the patient's medical records.

These requirements must be met in order to qualify for coverage under the “Limitations” section of LCD L33398.
- Limitations to be considered.
As discussed in LCD L33398, providers must carefully assess the benefits to be derived from the use of transcranial magnetic stimulation. The benefits of TMS use must be carefully considered against the risk of potential side effect in patients with any of the following:
- Transcranial magnetic stimulation is NOT considered reasonable and necessary in any of the following situations.

- Documentation requirements.

UPIC audits are focusing on your compliance with the LCD's documentation requirements. Are your Transcranial Magnetic Stimulation services fully documented?
- Utilization guidelines.

VI. How Can You Reduce Your Level of Regulatory Risk?
As discussed above, if your transcranial magnetic stimulation claims are targeted by a UPIC, the OIG or DOJ, the types of enforcement actions that can be pursued vary widely, depending the facts in your particular case. Unfortunately, since data mining is one of the primary ways that a potential target is identified for review, the first time that you know find out that your claims utilization practices are being assessed could be when you receive notice that your practice has been placed on prepayment review. In more serious cases, you may receive a OIG subpoena for records or a Civil Investigative Demand for records from the DOJ.
As a first step, if you have not already done so, you need to develop and implement an effective Compliance Program. Assuming that you already have such a program in place, take the time now, before you have a problem, to assess your care and treatment practices. Does your documentation meet applicable requirements? Have you documented that the care and treatment decisions made were medically necessary and appropriate? Were the services properly coded and billed?
VII. Responding to an Audit of Your Transcranial Magnetic Stimulation Claims:
- Learning of a prepayment or postpayment audit.
If your practice is placed on prepayment review, you will likely learn of the action through the electronic claims status system maintained by your MAC. Providers are normally given 45 days to submit the requested supporting documentation to their UPIC. Should you fail to submit the requested documentation to the UPIC in a timely fashion, the very least that will happen is that your claims will be denied. As set out under the Section 1815(a) of the Social Security Act:“...no such payments shall be made to any provider unless it has furnished such information as the Secretary may request in order to determine the amounts due such provider under this part for the period with respect to which the amounts are being paid or any prior period.”
- Don’t turn an administrative audit into a civil or criminal case.
In cases where a provider repeatedly ignores a request for records (or fails to submit the supporting documentation within the allotted time period), a UPIC will likely make a referral to the OIG for investigation and review. Unfortunately, such a referral significantly raises the level of risk that a provider may face. Depending on the OIG’s findings, a provider may be assessed Civil Monetary Penalties or even be excluded [9] from participation in Federal and State health benefits programs. Additionally, if evidence of fraud or other improper conduct is identified, the case may be referred to the DOJ for civil action and / or criminal prosecution.Moreover, once a problem has been discovered, a physician can significantly complicate matters by concealing the problem, destroying evidence or falsifying records. Under various Federal obstruction statutes, a physician may be charged with obstruction of justice for willfully engaging in activities that obstruct, mislead, deceive, or impede a health care fraud investigation.
- Engage qualified, experienced health law counsel.
Unfortunately, the days when a practice could feel comfortable directly handling a medium to large-sized audit, without assistance from legal counsel are becoming fewer and fewer each year. There are a number of strategies that legal counsel may employ in an effort to minimize a physician’s possible exposure and liability. Call an experienced health lawyer and ask him or her to walk you through the process. If the attorney hasn’t handled these cases on a regular and repeated basis, talk to another firm.

- [1] For additional information on how your claims may have been targeted for audit, please see the following related article, please see Physicians Being Placed on Non-Random Prepayment Review in Unprecedented Numbers. Are You Ready for an Audit?
- [2] Medicare Program Integrity Manual, Chapter 3 - Verifying Potential Errors and Taking Corrective Actions. Section 3.4 Prepayment Review of Claims.
- [3] See MPIM Section 3.4.A.
- [4] Referrals to law enforcement are typically made to the Department of Health and Human Services, Office of Inspector General (OIG) and / or the U.S. Department of Justice (DOJ).
- [5] CPT Code 90836 is an add-on code for individual psychotherapy, insight oriented, behavior modifying and/or supportive, 45 minutes with the patient and/or family member (time range 38-52 minutes) when performed with an evaluation and management service.
- [6] This Evaluation and Management (E/M) code is used when billing for an “office or other outpatient visit for the evaluation and management of an established patient, which requires at least two of these three key components: a detailed history, a detailed examination and medical decision making of moderate complexity.”
- [7] As set out in Medicare’s program integrity guidance, “An LCD is a decision by a Medicare administrative contractor (MAC) whether to cover a particular item or service on a MAC-wide basis in accordance with Section 1862(a)(1)(A) of the Social Security Act (i.e., a determination as to whether the item or service is reasonable and necessary).” See MPIM 13.1.3. an issuance published by a MAC setting out coverage parameters for a particular service. The LCD only applies to providers in states included in the MAC’s jurisdiction. Having said that, if a particular jurisdiction does not have an LCD addressing a certain service, LCD guidance published by other MACs is often cited as persuasive (but not binding) authority. The requirements set out in an LCD must be consistent with all applicable laws, regulations, and national policies for coverage, payment, and coding. LCDs may address a specific clinical topic using procedure codes to define one or more treatments and using diagnostic codes to describe the clinical indications that would make the treatment(s) reasonable and Social Security Act § 1862(a)(1)(A), 42 U.S.C. § 1395y(a)(1)(A). necessary. For example, an LCD may limit coverage of an item or service to specific diagnoses, or it may prohibit coverage of an item or service completely. The coverage policy created by an LCD is applicable only in States within a contractor’s jurisdiction.
- [8] NGS’s LCD guidance for Transcranial Magnetic Stimulation services is covered in LCD L33398. This guidance applies to all services performed on or after June 15, 2018.
- [9] For instance, under 42 USC §1320a-7(b)(6), an individual or entity can be excluded for a minimum of a year if found have submitted claims for excessive charges, unnecessary services or services which fail to meet professionally recognized standards of care.
