 (October 16, 2019): A Federal District Court Judge recently sentenced a Murfreesboro, TN dentist to prison and ordered that he pay restitution to TennCare (Tennessee’s Medicaid program). Regrettably, the types of improper billing practices cited by the government in the criminal Information filed against the defendant dentist aren’t that uncommon. This recent prosecution serves as an excellent case study of why it is essential that dentists and dental practices take steps to ensure that their medical necessity, documentation, coding and billing practices fully comply with applicable regulatory requirements and contractual obligations. In addition to reviewing the types of improper conduct that led to the government’s criminal pursuit of the defendants in this case, this article examines how a Special Investigations Unit dental audit (SIU dental audit) by auditors and investigators at DentQuest, Delta Dental and Cigna can ultimately lead to a referral to State or Federal law enforcement officials. Once a referral is made, you and your dental practice may be subject to criminal investigation and prosecution.
(October 16, 2019): A Federal District Court Judge recently sentenced a Murfreesboro, TN dentist to prison and ordered that he pay restitution to TennCare (Tennessee’s Medicaid program). Regrettably, the types of improper billing practices cited by the government in the criminal Information filed against the defendant dentist aren’t that uncommon. This recent prosecution serves as an excellent case study of why it is essential that dentists and dental practices take steps to ensure that their medical necessity, documentation, coding and billing practices fully comply with applicable regulatory requirements and contractual obligations. In addition to reviewing the types of improper conduct that led to the government’s criminal pursuit of the defendants in this case, this article examines how a Special Investigations Unit dental audit (SIU dental audit) by auditors and investigators at DentQuest, Delta Dental and Cigna can ultimately lead to a referral to State or Federal law enforcement officials. Once a referral is made, you and your dental practice may be subject to criminal investigation and prosecution.
I. SIU Dental Audit Reviews by DentaQuest, Delta Dental and Cigna Can Result in a Referral to State or Federal Law Enforcement Officials
In this case, a Tennessee licensed dentist reportedly owned a dental practice with three locations in Murfreesboro, TN and a single location in Lebanon, TN. The dental practice treated patients that were covered by private-payor dental plans and Medicaid. Payors billed by the dental practice included, but were not necessarily limited to: DentaQuest (DentaQuest served as the administrator to the TennCare program – Tennessee’s Medicaid program), Delta Dental and Cigna [1]. Starting in late 2014, a number of payors initiated an SIU dental audit of the defendant's multi-location dental practice. These included:
December 2014 DentaQuest SIU Dental Audit. In late 2014, DentaQuest conducted an audit of select 2013 and 2014 claims submitted to the Medicaid payor plan by the practice. After reviewing the claims, DentiQuest alleged that the practice claiming was:
- Billing for crowns at an unusually high rate; and
- Impermissibly billing DentaQuest for services provided by non-credentialed dentists.
Importantly, the defendant was allegedly advised of these allegations both during and after the DentaQuest audit.
December 2016 Delta SIU Dental Audit. Delta Dental conducted an audit of 2015 and 2016 claims submitted to the payor for coverage and payment. At the conclusion of the dental claims audit, Delta Dental alleged that the dental practice:
- Billed for dental services during the period January 2015 through May 2016 that were allegedly not provided.
Both during and after the Delta Dental audit, the defendant dentist and his office manager were allegedly advised of the allegation that the practice had billed the payor for services that were not provided.
August 2016. Tennessee Bureau of Investigation Probe.In August 2016, the defendant dentist and his office manager reportedly learned that the Tennessee Board of Investigation had initiated an investigation of the dental practice’s billing conduct. Despite the fact that the defendants supposedly learned of the State’s ongoing investigation, they allegedly:
- Directed employees to continue to bill for work that had not been performed.
As the summary findings of these dental claims audits reflect, the defendant dentist and the practice administrator were repeatedly advised by dental plan sponsors that a number of medical necessity, coding and documentation deficiencies had been identified. Despite the fact that the defendants were allegedly put on actual notice of these improper coding and billing practices, the practice appears not to have taken remedial steps to correct the conduct.
II. Overview of the Fraudulent Dental Billing Conduct Alleged by the Government
The criminal Information filed against the defendant dentist outlines a number of documentation and billing practices that allegedly resulted in the submission of false and fraudulent dental claims to the DentaQuest (TennCare Medicaid), Delta Dental and Cigna payor plans. Not surprisingly, the types of improper conduct that the government chose to criminally prosecute are far from uncommon. In fact, many of the dental audits we have defended on behalf of dental practices around the country have involved at least one of the documentation, coding and / or billing problems that ultimately led to the criminal referral in this case. As both government and private payor SIU dental audit representatives will readily attest, when it comes to dental claims fraud, the old adage “. . . there is nothing new under the sun” certainly applies [2]. The types of improper conduct alleged by the government are outlined below:
| Summary of Allegation | Conduct Cited by the Government |
|---|---|
| Billing for Services Not Rendered. | The government alleged that the defendants submitted false and fraudulent claims to health care benefit programs for dental work that had not been completed. |
| Falsifying Dates of Service. | The government alleged that the defendants falsified the dates of service to make it appear as though the dental service was rendered within the timeframe required by a health care benefit program or after preauthorization was obtained from a health care benefit program so that the dental claims would be paid. |
| Falsifying the Identity of the Individual Who Rendered the Dental Services. | The government alleged that the defendants falsified claims to make it appear as though the services had been rendered by a dentist who was credentialed to treat patients at a particular practice location, when in fact the services had been provided by a non-credentialed dentist or at a different practice location [3]. |
| Falsifying Dental Records. | The government alleged that the defendants falsified supporting documentation and records, such as x-rays, in order to have the claims paid. |
| Engaging in Upcoding. | The government alleged that the defendants added false language to the claim narratives to make it appear as though the practice had provided more expensive services than the services that were actually provided. |
| Obstruction. | The government alleged that the defendants falsified took steps to conceal the fraud, including: (1) Disciplining or firing employees who asked questions about whether the billing practices were correct or legal, (2) Instructing practice employees to tell patients and representatives from insurance companies that if the practice had billed for work that had not been done, it was simply a billing error and would be corrected, when, in fact, it was the routine practice of the organization. |
| False Statements / Obstruction. | The government alleged that the defendants falsified took steps to make it appear as though the practice administrator was solely responsible for the fraudulent billing practices at the practice and that the defendant dentist was supposedly unaware of the fraudulent billing practices, when in fact, both individuals knew about the conduct and caused the practice to submit false and fraudulent claims. |
III. Criminal Charges Brought Against the Defendant Dentist and Disposition of the Case
The defendant dentist in this case entered into a plea bargain with the Federal government and agreed to waive his right to an Indictment. As the pleadings in this case reflect, in November 2018, the defendant dentist was charged in a criminal Information with one count of criminal conspiracy under 18 USC § 1349 [4]. In June 2019, the defendant dentist was sentenced to almost three years in prison and ordered to pay almost one million dollars in restitution to the TennCare Medicaid program [5].
How can you and your dental practice avoid engaging in the types of improper conduct identified by the government in this case? As a first step, your practice needs to develop, implement and adhere to the both the letter and the spirit of an effective compliance program. An overview of the compliance program process is set out below.
IV. Every Dental Practice Must Develop and Implement an Effective Compliance Program
As you will recall, the Department of Health & Human Services (HHS), Office of Inspector General (OIG), issued voluntary Compliance Guidance for Individual and Small Group Physician Practices” almost 20 years ago, in 2000 [6]. As the seven element compliance guidance reflects, the term “physician” is defined to include “a doctor of dental surgery or dental medicine.”[7] With the passage of the Affordable Care Act [8] in 2010, dental practices and other health care providers participating in Federal health benefits programs were now required to establish a compliance program as a condition of their enrollment in the Medicare, Medicaid, and Children’s Health Insurance Program (CHIP) payor plans. Under § 6401(b)(5) of the statute:
“Subtitle E—Medicare, Medicaid, and CHIP Program Integrity Provisions
SEC. 6401. PROVIDER SCREENING AND OTHER ENROLLMENT REQUIREMENTS UNDER MEDICARE, MEDICAID, AND CHIP.Sec. 6401(a)(7): COMPLIANCE PROGRAMS.—On or after the date of implementation determined by the Secretary under subparagraph (C), a provider of medical or other items or services or supplier within a particular industry sector or category shall, as a condition of enrollment in the program under this title [Medicare], title XIX [Medicaid], or title XXI [CHIP], establish a compliance program that contains the core elements established under subparagraph (B) with respect to that provider or supplier and industry or category.
. . . .Sec. 6401(b)(5): COMPLIANCE PROGRAMS.—The State requires providers and suppliers under the State plan or under a waiver of the plan to establish, in accordance with the requirements of section 1866(j)(7), a compliance program that contains the core elements established under subparagraph (B) of that section 1866(j)(7) for providers or suppliers within a particular industry or category.” (emphasis added).
From a practical standpoint, dental practices have been slow to make the transition from a “voluntary” to a “mandatory” approach towards compliance. In January 2017, the OIG and compliance professionals of the Health Care Compliance Association (HCCA) met and made modifications to the original seven elements identified in the 2000 compliance program guidance. The seven elements were modified to include the following:
- Standards, Policies, and Procedures.
- Compliance Program Administration.
- Screening and Evaluation of Employees, Physicians, Vendors and other Agents.
- Communication, Education, and Training on Compliance Issues.
- Monitoring, Auditing, and Internal Reporting Systems.
- Discipline for Non?Compliance.
- Investigations and Remedial Measures [9].
If the defendants had properly developed, implemented and diligently worked to follow an effective dental practice compliance program, it is highly unlikely that the deficiencies identified by the government would have occurred (assuming, of course, that the defendants would have worked to comply with applicable statutory and regulatory requirements).
V. The Possible Impact of an SIU Dental Audit on Your Dental Practice
Assuming that your dental practice does not participate in the Medicare program [10] (but does participate in the Medicaid program), a wide variety of audit entities may show up at your door to perform an “unannounced audit” or send you a written notice of audit. Audit entities that may initiate a review of your dental claims include:
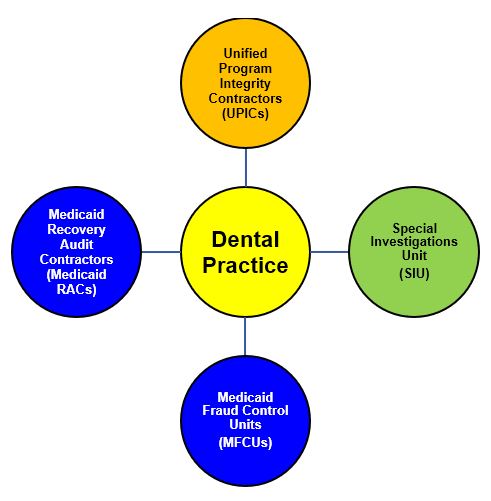
It is important to keep in mind that many of these audit entities have overlapping areas of responsibility. As a result, it is entirely possible that one audit entity (for instance, a Unified Program Integrity Contractor (UPIC)) may decide to look at your 2015 Medicaid dental claims, while a completely different entity (such as Medicaid Recovery Audit Contractor (Medicaid RAC)) could audit your 2016 Medicaid dental claims. For instance:
- UPIC / Medicaid RAC Audits. On the government side, your dental practice’s Medicaid claims may be audited by a UPIC or a Medicaid RAC working for the Centers for Medicare and Medicaid Services (CMS).
- State MFCU Audits. Since the Medicaid program is jointly funded by the Federal and State governments, your Medicaid claims may also be audited by your State’s Medicaid Fraud Control Unit (MFCU).
- Audits by a Private Company Administrator of the Medicaid Program. If a private payor plan (such as DentaQuest) is serving as the administrator of the State Medicaid program, the private payor Special Investigations Unit (SIU) may initiate an audit of your Medicaid claims
- Private Payor Audits. To the extent that your dental practice is a participating provider in one or more private dental payor plans, each of these private payor plans has an in-house SIU that is tasked with identifying and taking appropriate administrative action against providers and suppliers engaged in improper conduct. If a SIU identifies conduct that it believes may constitute fraud, it may choose to make a referral to law enforcement for further investigation and possible criminal prosecution.
In the case discussed above, the Special Investigation Units (SIU) of DentQuest, Delta Dental and Cigna initiated audits of the dental practice’s claims. A private payor’s SIU is typically comprised of health care auditors and investigators, many of whom previously worked for Federal or State law enforcement agencies. If evidence of wrongdoing is found by the SIU, the private payor may decide to take an administrative action, such as place a dental provider on prepayment review or terminate a dental provider from their payor program. To the extent that an alleged overpayment is identified by the SIU, it may send a demand letter to a dental provider. This ultimately could lead to the initiation of a collection action in civil court by the private payor. In a worst case scenario, if an SIU agent identifies evidence of actual fraud (as opposed to conduct that is indicative of a mistake, error or an accident), the unit may choose to make a referral to the government for further investigation and possible criminal prosecution.
As set out in the background discussion (Section I), the dental practice in the instant case underwent several audits over a fairly short period of time. The audits conducted included reviews by DentaQuest (as the administrator for TennCare’s Medicaid dental program), Delta Dental and Cigna. The Tennessee Bureau of Investigation subsequently initiated its own investigation of the dental office’s billing practices. After concluding their reviews, a criminal referral was made to the U.S. Attorney’s Office. Federal prosecutors then initiated criminal proceedings against the dentist practice owner and the practice administrator.
VI. Responding to a DentaQuest Audit, Delta Dental Audit or Cigna Audit of Your Dental Claims
The government does not expect you to be perfect with respect to your documentation, coding and billing practices. Nevertheless, the government does expect you to take reasonable steps to prevent the occurrence of improper billing practices. The development and implementation of an effective compliance program is an integral part of your dental practice’s program integrity efforts. Unfortunately, even if you diligently work to stay within the four corners of the law, mistakes will still be made and your dental claims will still be subject to audit by a State Medicaid program, DentaQuest, Delta Dental, Cigna and other dental payors. How should you respond if you are audited by a government or private payor?
- Call an Experienced Health Lawyer for Assistance. Effectively responding to a government or private payor audit of your dental claims is essential if you hope to reduce the possible adverse effects of an audit. An experienced health lawyer can walk you through the process and interact directly with the payor to seek an extension of the deadline to submit dental records and advise you on the documentation, coding and billing requirements that are required by a given payor. Notably, the Liles Parker attorneys who would represent you and your practice in a dental audit are both experienced health lawyers AND have achieved certification as Certified Medical Reimbursement Specialists (CMRSs) by the American Medical Billing Association (AMBA) and / or Certified Professional Coders (CPCs) by the American Academy of Professional Coders.
- Don’t ignore a SIU dental audit of your claims. It has been our experience that approximately 20% of all dental audit requests are either ignored by a dental practice or were set aside for later review and then got lost in the ever-growing pile of administrative correspondence received by a dental practice. Don’t allow this to happen. Most payors will give a dental practice a deadline to submit any responsive, supporting dental records. This submission deadline can be as little as a few days to as much as 30 days. If the payor does not receive the requested records by the deadline, it will automatically deny the dental claims.
- Are there indications that the government or private payor intends to try and extrapolate damages? If a payor describes the group of dental medical records requested as a “statistically relevant sample” or uses similar descriptive terminology, call your legal counsel. While not typically seen in private payor audits, we have seen numerous instances where a private payor has attempted to extrapolate any damages identified in connection with their audit. Depending on applicable law and the terms of your contract with the payor, your legal counsel may be able to get the extrapolation dismissed. If the payor does, in fact, have the authority to extrapolate damages, Liles Parker attorneys will often work with a statistical expert to conduct a preliminary assessment of whether or not the sample selected is, in fact, a sample that is representative of the universe of dental claims at issue.
- Assemble the dental records requested. Take the time to assess the specific claims at issue and the supporting documentation in each file. Are there additional places (e.g., files in storage) where additional supporting documentation may be kept? If the documentation appears to be incomplete, you may be able to supplement the records with an affidavit. Are there any referring or ancillary providers that might have supporting documentation (e.g., referrals or orders from another dental professional, laboratory or X-ray test result)?
- Retain duplicates of any information that you submit to the SIU dental auditor. Should you choose to go it alone and not be represented by legal counsel, you need to make sure that you secure a complete copy of the documentation sent to the payor. It should be kept separate from your working files. Should an appeal prove necessary, you will need to know the information on which the payor based its denial decision.
- Don’t turn an administrative or civil audit into a criminal case. Dental records, progress notes, x-rays and other documents must be signed and dated by the health care provider at the time the services are rendered or conducted. In conducting your review, did you find that the claims documentation is legible and complete? If not, change your practices now. Wholesale efforts to go back and supplement incomplete documentation may constitute obstruction of justice if incorrectly handled. Never make changes to a patient’s documentation or dental records without first discussing the issues presented with legal counsel so that you can ensure that a third party reviewing the updated records will not be misled as to the nature of the changes or revisions AND when the changes or revisions were made. In other words, your records must accurately show when changes, corrections or additions were made to the patient’s dental records. Late entries to a record must be dated as such. More than likely, government and private payor auditors will give very little (if any) credit to late entries or supplemental records unless the service being supplemental was recently performed. The falsification of information in a patient’s dental record (or in other records presented to the government, its agents or private payor auditors) can constitute a criminal violation and could lead to much bigger troubles for you and your dental practice than a mere overpayment.
Private payor SIUs are an important source of referrals for State and Federal prosecutors. Your compliance with a payor’s medical necessity, documentation, coding and billing requirements will be carefully reviewed by a SIU if your dental claims are subjected to an audit by the payor’s anti-fraud unit. If evidence of criminal fraud is identified, there is real possibility that your conduct will be referred to the government for further investigation and possible prosecution. Your adoption and implementation of an effective compliance program will greatly reduce your level of risk. Liles Parker attorneys have extensive experience working with dental practices around the country to develop and implement an effective compliance program. Part of this process includes the performance of a “GAP Analysis” to determine whether the practices current practices are consistent with applicable regulatory and contractual requirements. If deficiencies are identified, remedial steps can then be taken to bring the practice back into compliance.

Is your dental practice being audited by DentaQuest, Delta Dental or Cigna? If so, give us a call. We can help. A number of Liles Parker attorneys are experienced defending dental practices in Medicaid and private payor audits. Moreover, these attorneys are both experienced health lawyers AND Certified Professional Coders (CPCs). For a free consultation, please give us a call: 1 (800) 475-1906
- [1] Each of these plans qualify as “health care benefit programs” as defined by 18 USC § 24(b).
- [2] Ecclesiastes 1:9 reads, in part “What has been is what will be, and what has been done will be done again. There is nothing new under the sun.”
- [3] Are Your Providers Properly Credentialed with Each Payor? How long does it take for the payor to credential a new dentist? Once a new dentist is approved, will the payor cover dental claims back to the submission date of credentialing package? We are seeing a huge rise in the number of overpayments based on failure to credential. A detailed discussion of this credentialing issue is discussed in an article entitled: “The Dangers of Billing Payors for the Services of a Non-Credentialed Dentist / Non-Participating Dentist.”
- [4] Under the Fifth Amendment of the Constitution, a criminal defendant in a Federal case has a constitutional right to be indicted by a Grand Jury. An Information is typically used by the government when a defendant voluntarily pleads guilty (typically after entering into plea bargain negotiations with the government).
- [5] Notably, the defendant practice administrator has not entered a guilty plea and is scheduled to be tried in December 2019.
- [6] 65 Fed. Reg. 59434. (October 5, 2000).
- [7] 65 Fed. Reg. 59434, 59435.
- [8] A copy of the Affordable Care Act can be found at the following link: https://www.govinfo.gov/content/pkg/PLAW-111publ148/pdf/PLAW-111publ148.pdf
- [9] See “Measuring Compliance Program Effectiveness – A Resource Guide.”
- [10] Generally speaking, traditional Medicare does not cover most routine dental care procedures, such as cleanings, fillings, tooth extractions, dentures, or other common dental procedures. Under certain circumstances, Medicare Part A may cover dental services that are needed in connection with the provision of a covered Part A service (e.g. an operation your jaw). Additionally, some Medicare Advantage are now starting to cover a limited scope of routine dental procedures.

You must be logged in to post a comment.