(August 4, 2022): Over the past year, we have seen a significant increase in the number of Medicare administrative audits, False Claims Act investigations and criminal prosecutions by the Department of Justice (DOJ), related to the billing of allogeneic (harvested from someone else) stem cell products. Medicare and Medicaid claims stemming from amniotic liquid and amniotic membrane tissue “stem cell” products have garnered significant scrutiny from law enforcement currently being investigated by the government and private payors around the country. We will also discuss how these cases have arisen and the steps that you can take to reduce your level of risk.
I. Amniotic Liquid / Amniotic Membrane Tissue Products -- Description and Treatments:
Simply stated, when a baby is still in its mother’s womb, it is encased in a fluid-filled sac. The fluid filling the sac is known as “amniotic fluid.” [1] The walls of this fluid-filled sac are known as the “amniotic membrane.” [2] As part of the birthing process, the amniotic membrane breaks (this is colloquially referred to as the mother’s water breaking) and the mother goes into labor. When the amniotic membrane breaks, it may be possible to collect the amniotic liquid that is released. In recent years, amniotic fluid and membrane-based products have been actively marketed by medical companies for use in the treatment of a wide variety of illnesses and conditions. In some cases, the various potential clinical applications of these products have been widely extolled by sales representatives around the country.
II. Stem Cell Therapies Using Amniotic Fluid / Amniotic Membrane Tissue Products:
Despite all the hype surrounding their potential clinical applications, stem cells truly are amazing. Stem cells are highly specialized human cells that have the potential to develop into many different cell types, ranging from muscle cells to brain cells. While stem cell therapies are currently all the rage, it is worth noting that they were first used in 1958 by George Mathe, a French Oncologist, who performed stem cell transplants of bone marrow grafts to treat six nuclear scientists who had been accidentally exposed to radiation.[3] Today, the number of companies researching, and marketing stem cell treatment applications is ever-expanding.
The U.S. Food and Drug Administration (FDA) is responsible for regulating regenerative medicine products (such as stem cell products). In November 2017, the FDA first issued guidance[4] covering the development and oversight of regenerative medicine products. Based on the November 2017 guidance, the FDA determined that amniotic fluid falls under Section 351 of the Public Health Service (PHS) Act. As such, they would require an approved Biologics License Application prior to marketing. In the absence of such a license, the selling and marketing of amniotic fluid products may be problematic.
The FDA has expressly noted that some regenerative stem cell products have been illegally marketed, are not effective, and in cases may pose significant patient safety issues.[5] In fact, since December 2019, the agency has issued more that 350 letters to manufacturers, clinics and health care providers cautioning them about offering unapproved regenerative medicine products.[6] This is especially troubling in the case of amniotic fluid and membrane products. The problem is that although stem cells have been found in fresh amniotic fluids and membranes, the processing of these products effectively sterilizes the stem cells that may have been present. If any living stem cells remain, the amniotic product would be classified as a drug and would not be marketable until clinical trials are conducted. Therefore, any medical companies (or their marketing representatives) representing that their amniotic products contain living stem cells would be subject to FDA enforcement.
To be clear, even in the absence of living stem cells, amniotic fluid and membrane products may still be helpful in the cell regenerative process. For example, amniotic fluids contain collagen, extracellular matrix proteins, and growth factors which may promote the regenerative healing of tissue. Today, a number of liquid amniotic fluid allograft products have been marketed to treat ailments including sports injuries, tendonitis, joint pain, arthritis and osteoarthritis, and muscle or tendon tears. Unfortunately, these illnesses are not currently designated by the FDA as an approved condition for treatment. As the FDA noted in its July 2020 Consumer Alert, amniotic tissues had not been approved for the treatment of any orthopedic condition.
III. Medicare and Medicaid Coverage of Amniotic Liquid, Amniotic Tissue, Skin Substitute, and Wound Care Products:
-
Medicare Coverage of Amniotic Liquid Allografts.
A number of specific CPT codes[7] have been established for the injection of amniotic liquid allografts[8] into different parts of the body. Nevertheless, at this time, the Centers for Medicare and Medicaid (CMS) has not specifically approved the coverage of amniotic liquid allografts. Perhaps the final nail in the coffin for amniotic liquid allografts has been the fact that a covered procedure cannot be considered "experimental or investigational". Most payors still include Fluid Flow on their experimental and investigational list for all orthopedic conditions.[9] As policies are updated, some payors, like Blue Cross Blue Shield of Rhode Island,[10] are considering some uses of the product as medically reasonable. Hopefully, with more time, we may see a shift away from the product’s listing in the experimental category.
Currently, the coverage of amniotic liquid allograft treatment applications are still relatively new. There are only a few peer-reviewed studies regarding the efficacy of such products, especially in relation to other, more traditional treatments. Several published studies have shown marked improvement in treating osteoarthritis with liquid amniotic suspensions[11] compared to traditional methods. These studies could perhaps be referenced in an appeal to attest to the product’s necessity in treating osteoarthritis but are not applicable for any other treatment method utilizing liquid allografts. -
Medicare Coverage of Amniotic Tissue / Skin Substitute / Wound Care Products.
CMS has approved coverage amniotic membrane tissue and skin substitute products for various wound care applications. Applicable sets of Local Coverage Determination (LCD) guidance have since been updated (one as recently as February 2022) and now focus on amniotic membrane grafts. Relevant Medicare LCDs and articles associated with amniotic tissue products, including the following:
LCD L35041: Application of Bioengineered Skin Substitutes to Lower Extremity Chronic Non-Healing Wounds.
LCD L36690: Wound Application of Cellular and/or Tissue Based Products (CTPs), Lower Extremities.
LCD L36377: Application of Skin Substitute Grafts for Treatment of DFU and VLU of Lower Extremities.
Article A56155: Local Coverage Article -- Use of Amniotic Membrane Derived Skin.Upon examination of these LCDs and articles, it again becomes clear that CMS has focused its attention on amniotic membrane / skin substitute and wound care grafts rather than amniotic liquid allografts or other injectable tissue-based products. However, the LCD L36690 does briefly discuss FDA regulation of tissue-based products and thus may extend to liquid allografts. The LCD states the following:
“Evaluation of the clinical literature indicates that studies comparing the efficacy of CTPs to alternative wound care approaches with patients’ autologous skin are limited in number, apply mainly to generally healthy patients, and examine only a small portion of the CTP products available in the United States. Therefore, all products with FDA clearance / approval or designated 361 HCT/P exemption used in accordance with that product’s individualized application guidelines will be equally considered for the purpose of this LCD and may be considered reasonable and necessary.” (Emphasis added).
Though this may seem like a positive step for amniotic liquid allograft products, the FDA has not released any literature or made any indication that their stance on tissue-based products for pain management or orthopedic use has changed. If that is true, then the 2020 Consumer Alert previously described still applies today. At this time, amniotic tissue and skin substitute products are still only viable as a billable treatment when used for wound care. No orthopedic treatments or pain management is currently within the scope of coverage.
IV. Law Enforcement Has Initiated Medicare Audits of Amniotic Liquid / Amniotic Tissue / Skin Substitute / Wound Care Claims:
-
UPIC Audits of Original Medicare Part B Amniotic Tissue / Skin Substitute / Wound Care Claims.
Over the last year, CMS program integrity contractors (such as Unified Program Integrity Contractors (UPICs)), have ramped up their audit efforts with respect to amniotic tissue products, skin substitutes and other wound care products. It is important keep in mind that when a UPIC audits these claims, the audits will be conducted on two levels:
Level 1 UPIC Audits: At this initial level of review, UPICs will essentially dissect each claim amniotic tissue / skin substitute and / or wound care treatment and determine whether it meets all applicable requirements to qualify for coverage and payment. There are eight factors that will be examined by the UPIC, each of which are summarized in the chart below:
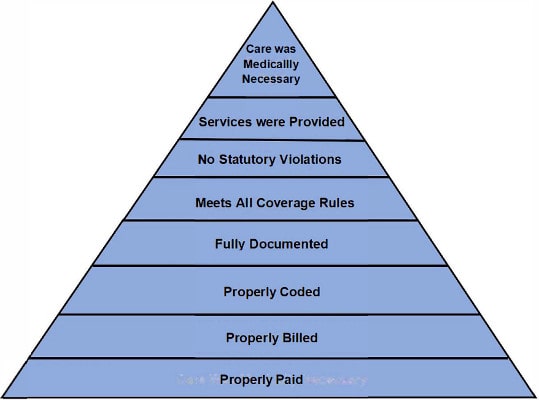
Generally, these requirements are referred to as the “Eight Elements of a Payable Claim.” To assess these eight elements, UPICs have been requesting an enormous amount of information from billing providers, literally asking for documents ranging from a completed patient “Beneficiary Notice of Liability” form to detailed wound care evaluation and treatment documentation.
Of the eight elements, properly documenting “Medical Necessity” is the element where many providers come up short. In order to show medical necessity, there are several less invasive, less costly, more conservative methods of treatment that payors will expect to see evidence that they were attempted (and failed) before a tissue product or skin substitute may be considered. These predicate treatment approaches include—but are not limited to—rest, ice, stretching, physical therapy, and splints or braces. With respect to documentation standards for a related tissue product / skin substitute graft procedure, LCD L36690 states:
“Documentation (in the pre-service record) specifically addressing circumstances as to why the wound has failed to respond to standard wound care treatment of greater than 4 weeks and must reference specific interventions that have failed. Such record should include updated medication history, review of pertinent medical problems that may have occurred since the previous wound evaluation, and explanation of the planned skin replacement surgery with choice of CTP [tissue product] graft product. The procedure risks and complications should also be reviewed and documented.” (Emphasis added).
Further, to comply with the standards of reasonableness and necessity, a service must adhere to the definition of the terms as seen in CMS IOM 100-08, Chapter 13, Section 13.5.1.[12]
Level 2 UPIC Audits: In addition to performing a traditional analysis of the medical necessity, documentation, coding and billing aspect of each wound care claim, UPICs are also carefully examining the business side of wound care treatment and management. For example, recent UPIC audits have asked for skin substitute and wound care product inventory logs (including lot numbers); copies of all invoices for invoices for skin substitute and wound care products; documentation related to any rebates issued by distributors or manufacturers in connection with skin substitute and wound care products; and copies of any marketing materials presented to the provider or to patients for skin substitute and wound care products.
-
Audits of Medicare Advantage (Part C) and Prescription Drug Plan (Part D) Amniotic Fluid Claims.
Last August, CMS’s Center for Program Integrity issued an alert to all Medicare Advantage Organizations (MAOs) and Prescription Drug Plan Sponsors (PDPs), warning them of questionable billing practices involving several Q codes related to amniotic tissue injections using human cell and tissue products. As the alert outlined, CMS has seen a steep increase in the billing of Q codes related to amniotic tissue injections for indications other than wound healing. Based on this alert, health care providers billing Medicare Advantage plans for amniotic tissue / skin substitute and wound care treatments should carefully review their medical necessity, documentation, coding and billing practices to better ensure that they are fully compliant with applicable regulatory and administrative requirements.
-
Criminal Prosecution of Misleading Amniotic Fluid Claims.
Two months ago (June 2022), a Physician Assistant in the Western District of Missouri was prosecuted and convicted in the Western District of Missouri of 10 counts of wire fraud and 10 improper drug distribution counts. The underlying conduct related to these counts varied, but one issue in particular is relevant to this article. The government alleged that the defendant marketed and administered “stem cell” amniotic fluid treatments to patients. As discussed previously, processed amniotic fluid doesn’t contain any “living” stem cells. The amniotic fluid product the defendant obtained from her distributor (the University of Utah) was a “sterile, filtered amniotic allograft. . . The amniotic fluid allograft was “acellular,” meaning it did not contain any cells, including stem cells.” It is worth noting that the government’s investigation was supposedly prompted by the Physician Assistant’s false and misleading statements made by the defendant’s statements to Springfield television station.
V. Closing Thoughts:
Regrettably, the hope and promise of stem cell therapy has emboldened a small number of health care providers, marketers, sales representatives, distributors and manufacturers to promote amniotic liquid allografts, amniotic tissue and skin substitute products in misleading ways. Health care providers using these products in the care and treatment of their patients must exercise caution when using these products. More specifically, health care providers should:
- Don’t rely on coverage statements or representations from sales representatives, marketers or distributors. Don’t assume that third parties trying to sell you their products know if it qualifies for coverage and payment by Medicare. Even assuming that a sales representative sincerely believes a product is covered for a specific indication (such as pain management), payor policies change. The sales representative may just be wrong. Therefore, conduct your own due diligence. Pull applicable LCDs and Medicare Coverage Articles so that you can verify what a payor’s current requirements for coverage and payment. Still unsure? Call an experienced health lawyer (preferably one who is also a Certified Professional Coder (CPC)) for assistance.
- Don’t be a cowboy. Think twice before using amniotic liquid or amniotic tissue products for an indication or diagnosis that has not been approved by the FDA. The FDA doesn’t regulate the practice of medicine, nor does it control the ordering or prescribing practices of physicians once an FDA covered product becomes available on the market. Perhaps the best example of this is the off-label use of drugs. Setting aside possible malpractice liability risks and claims coverage concerns, a physician is within his or her authority to prescribe medications for diagnoses and conditions that have not yet been recognized as an approved, covered medical condition by the FDA. Similarly, as long as it is in the best interest of a patient, a physician is permitted to order and use amniotic liquid and / or amniotic tissue products in the treatment of a medical condition that has not yet been expressly approved by the FDA. Having said that, just because a physician believes that an off-label use of an amniotic liquid or an amniotic tissue product is medically necessary does not mean that it will qualify for coverage and payment.
- Keep accurate records of your purchases. To the extent that a False Claims Act or criminal investigation of your wound care or skin substitute claims is initiated by the government, one of the first things that the government will do is compare the number of claims your practice has billed to Federal and private payors against the number of wound care and skin substitute products you have actually purchased. Additionally, if you have entered into any rebate agreements, you need to ensure that any rebates issued have been properly disclosed to Medicare and other Federal payors when billing for related claims. You should also maintain a copy of the rebate contract.
- Take audits and investigations seriously. Please remember – there is no such thing as a “random audit". If your dermatology or wound care practice receives an audit request from a Medicare Administrative Contractor (MAC) or UPIC, it is essential that you contact qualified health law counsel to assist you in responding to the audit. Similarly, if you receive notice of an investigation by the Office of Inspector General (OIG) or the Department of Justice (DOJ), you should refrain from making any statements until you have an opportunity to discuss the matter with an experienced health law attorney. Remember, everything you say is evidence.
Is your dermatology or wound care practice being audited or under investigation by the government? For a complimentary consultation regarding your case, please give us a call at: 1 (800) 475-1906

- [1] Human Cellular and Tissue-Based Products (HCT/Ps) defined at 21 C.F.R. §1271.3(d) as "articles containing or consisting of human cells or tissues that are intended for implantation, transplantation, infusion, or transfer into a human recipient." As set out in 21 C.F.R. §1271.3(d)(3), the definition of HCT/P expressly excludes "[s]ecreted or extracted human products, such as milk, collagen, and cell factors, except that semen is considered an HCT/P." The FDA has taken the position that amniotic fluids (secreted body fluids), are generally not considered HCT/Ps and are therefore NOT subject to 21 C.F.R. Part 1271. Although not an HCT/P, as a general matter, amniotic fluid intended to treat diseases or conditions in humans would be regulated as a drug and biological product under Section 351 of the Public Health Service (PHS) Act which defines a biologic product as "virus, therapeutic serum, toxin, antitoxin, vaccine, blood, blood component or derivative, allergenic product, or analogous product, … applicable to the prevention, treatment, or cure of a disease or condition of human beings." Many biological products subject to the PHS Act also meet the definition of drugs under the Federal Food, Drug and Cosmetic Act (FDC Act) and the FD&C Act and would be subject to premarket review and approval requirements. See the FDA’s guidance entitled "Frequently Asked Questions About Therapeutic Biological Products," dated July 7, 2015. Also see Letter dated November 10, 2020, from the FDA to Regenerative Cell Institute, LLC.
- [2] As further set out in the FDA's November 10, 2020 letter to Regenerative Cell Institute, LLC. ". . . allogeneic stem cell products derived from umbilical cord blood or amniotic membrane and intended to treat diseases or conditions in humans would be regulated as drugs and biological products under section 351 of the PHS Act and the FD&C Act and would be subject to premarket review and approval requirements." (Emphasis added).
- [3] Science News article, "The Beginnings of Stem Cell Therapy."
- [4] On November 15, 2017, the FDA first announced that it was issuing a comprehensive regenerative medicine policy framework.
- [5] The FDA has issued a Consumer Alert on "Regenerative Medicine Products Including Stem Cells and Exosomes." Issued July 22, 2020.
- [6] On April 21, 2021, the FDA issued guidance titled "Advancing the Development of Safe and Effective Regenerative Medicine Products."
- [7] Specific CPT Codes associated with liquid allografts currently being investigated include:
CPT Code 20550: Injection(s); single tendon sheath, or ligament, aponeurosis.
CPT Code 20551: Injection(s); single tendon origin/insertion.
CPT Code 20552: Injection(s); single or multiple trigger point(s), one or two muscles.
CPT Code 20553: Injection(s); single or multiple trigger point(s), three or more muscles.
CPT Code 20600: Injection(s); small joint.
CPT Code 20605: Injection(s); intermediate joint.
CPT Code 20610: Injection(s); large joint. - [8] An "allograft" is a tissue graft from a donor of the same species as the recipient. The donor and the recipient are not genetically identical. In contrast, an "autograft" is when a patient’s own tissue is used (for example, in a surgical reconstruction procedure).
- [9] See a list of Payor Medical Coverage Policies re: amniotic liquid allografts here
- [10] See a list of Payor Medical Coverage Policies re: amniotic liquid allografts here
- [11] Kimmerling, K.A., Gomoll, A.H., Farr, J. et al. Amniotic suspension allograft improves pain and function in a rat meniscal tear-induced osteoarthritis model. Arthritis Res Ther 24, 63 (2022). https://doi.org/10.1186/s13075-022-02750-9. See also Vines JB, Aliprantis AO, Gomoll AH, Farr J. Cryopreserved Amniotic Suspension for the Treatment of Knee Osteoarthritis. J Knee Surg. 2016 Aug;29(6):443-50. doi: 10.1055/s-0035-1569481. Epub 2015 Dec 18. PMID: 26683979 and Natali, S.; Farinelli, L.; Screpis, D.; Trojan, D.; Montagner, G.; Favaretto, F.; Zorzi, C. Human Amniotic Suspension Allograft Improves Pain and Function in Knee Osteoarthritis: A Prospective Not Randomized Clinical Pilot Study. J. Clin. Med. 2022, 11, 3295. https:// doi.org/10.3390/jcm11123295.
- [12] Retrieved from https://www.cms.gov/Regulations-and-Guidance/Guidance/Manuals/Downloads/pim83c13.pdf

You must be logged in to post a comment.